TL;DR / At-a-Glance Summary
Stipends Don’t Secure Devices
A healthcare mobile stipend does not guarantee a secure or compatible device. Hospitals still carry full HIPAA liability even when employees use personal phones.
BYOD Creates Hidden Risk
Unmanaged BYOD environments expose patient data through outdated phones, unsecured apps, and lost devices. Without MDM controls, healthcare organizations cannot enforce encryption or remote wipe.
Compliance Is Expensive
Healthcare data breaches now average $9.77M, and state reimbursement laws add financial exposure. Stipends shift device costs to employees but leave hospitals responsible for compliance failures.
CaaB Standardizes Mobility
Connectivity as a Benefit replaces stipends with MDM-enrolled, HIPAA-ready devices and managed connectivity. This improves nurse mobile access while giving IT teams visibility and control.
Spenza Enables CaaB
Spenza provides the infrastructure to deploy CaaB through a branded device portal, automated eSIM provisioning, and integrated telecom expense management. Hospitals can reduce mobile costs while maintaining secure, compliant connectivity.

Connectivity as a Benefit (CaaB) is a modern
mobile stipend solution that transforms the traditional
cash mobile stipend into a
managed, employer-sponsored program. Instead of giving employees money and relying on them to choose the right plan, CaaB provides access to
discounted mobile plans and optional
devices through a controlled, branded experience.
The program includes
governance,
reporting, and
automated settlement, offering a structured,
tax-advantaged solution that keeps employees connected while giving employers
visibility and control.
Healthcare runs on connectivity. From scanning medications at the bedside to charting vitals in an Electronic Health Record (EHR) system, millions of frontline healthcare workers in the United States rely on mobile devices for tasks that directly affect patient safety.
Nearly 80% of nurses now rely on smartphones for clinical communication and documentation. Yet most health systems still hand nurses and clinical staff a flat monthly stipend, typically $50 to $75, and hope for the best.
The result? Unmanaged personal devices accessing protected health information, outdated phones that crash mid-shift, and compliance gaps that can trigger HIPAA violations costing millions.
This blog explores why the traditional healthcare mobile stipend is broken, how unmanaged BYOD programs create serious compliance risk, and what a modern alternative called Connectivity as a Benefit (CaaB) looks like in practice.
You will also see a real-world ROI framework showing how a 5,000-nurse health system can cut its mobile spend from $3 million to $1.68 million while eliminating HIPAA risk, all powered by Spenza’s managed connectivity platform.
Key Takeaways:
- A $50 stipend does not guarantee a HIPAA-ready device. It simply shifts liability to the employee and risk back to the organization.
- Unmanaged BYOD in healthcare exposes patient data, violates state reimbursement laws, and increases nurse turnover.
- Connectivity as a Benefit (CaaB) delivers Mobile Device Management (MDM)-enrolled, HIPAA-compliant mobile devices with audit trails at roughly half the cost of traditional stipend programs.
- Spenza’s platform enables healthcare organizations to provision compliant devices through a branded portal with eSIM technology, SOC 2-ready infrastructure, and integrated telecom expense management.
A Day in a Nurse’s Shift: When Mobile Access Fails
Picture this. It is 6:47 a.m. and Sarah, an ICU nurse, arrives for her twelve-hour shift. She reaches for her personal phone to clock in through the hospital’s workforce management app. The screen freezes. She force-restarts, but the e-HR app will not load because her three-year-old phone no longer supports the latest OS update.
She borrows a colleague’s device to look up a medication dosage, inadvertently logging into the hospital’s secure messaging platform on someone else’s unmanaged phone.
In less than fifteen minutes, three things have gone wrong: a missed clock-in creating a payroll discrepancy, a delayed medication check that could compromise patient safety, and a potential HIPAA exposure because protected health information was accessed on a device with no remote-wipe capability.
Sarah is not careless. She is a dedicated clinician working within a system that gave her a $50 monthly stipend and told her to figure out the rest. Her situation is not unusual. It is the norm across American healthcare.
A nurse may use a phone to:
- Access patient charts through EHR apps
- Scan medications
- Communicate with physicians
- Clock in and manage shifts
- Receive emergency alerts
Yet many healthcare organizations still rely on a simple solution: a monthly mobile stipend.
This is where Connectivity as a Benefit for Healthcare is changing the conversation.
The Healthcare Mobile Stipend Problem
The stipend model was designed for simplicity. Give every employee a flat dollar amount, let them use their own phone, and move on. In an office environment with low regulatory stakes, this can work. In healthcare, it falls apart for three main reasons.
1. The math does not add up.
A reliable smartphone with a data plan adequate for clinical applications (EHR access, barcode scanning, secure messaging, telehealth) costs well north of $50 a month when you factor in device payments, insurance, and a data plan that will not throttle during a critical shift.
2. There is zero guarantee of device quality or security.
Some nurses will use a current-model iPhone with biometric authentication. Others will use a five-year-old Android that has not received a security patch in eighteen months. The hospital has no visibility into which devices are accessing its network, no ability to enforce encryption, and no way to remotely wipe a lost device containing patient data.
3. The financial exposure is enormous.
According to an analysis on the Cost of a Data Breach Report, the average cost of a healthcare data breach reached $9.77 million, the highest of any industry for the fourteenth consecutive year. A single unmanaged device lost in a parking lot can trigger an investigation, breach notifications to thousands of patients, and penalties that dwarf whatever the organization saved by choosing stipends over managed devices.
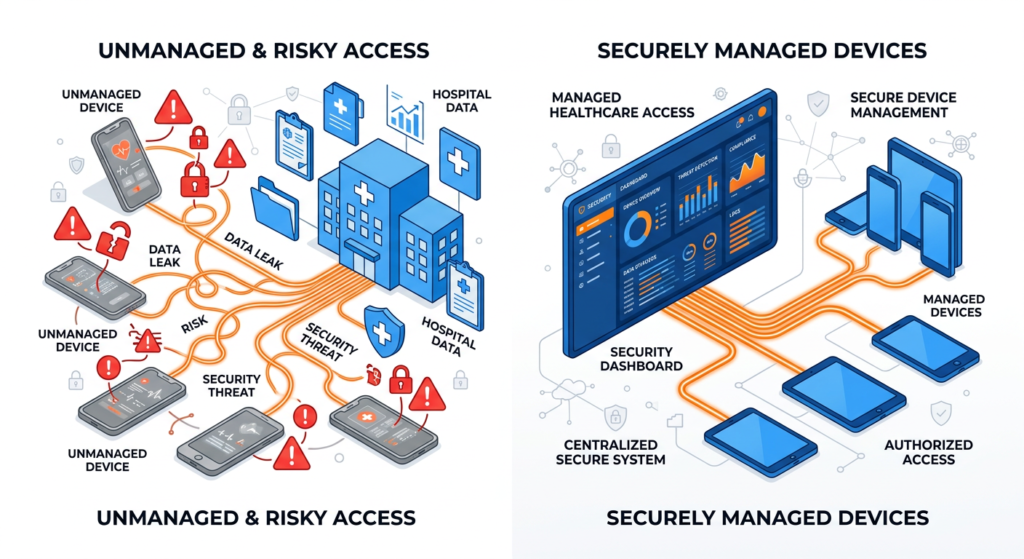
Why Mobile Stipends Fall Short
To better understand the limitations of stipend-based programs, the table below compares how traditional stipends differ from managed connectivity approaches used in modern healthcare environments.
| Issue | Stipend Model | Managed Connectivity |
|---|---|---|
| Device standards | Vary by employee | Standardized devices |
| Security control | Limited | Full IT oversight |
| App compatibility | Inconsistent | Pre-configured |
| Reliability | Depends on personal device | Enterprise-grade |
A stipend alone cannot ensure a secure device, reliable connectivity, or compliance with hospital policies. Because of this, frontline healthcare connectivity often becomes inconsistent.
HIPAA and BYOD: Why Unmanaged Devices Are a Compliance Bomb
Think of HIPAA compliance like the plumbing in a hospital. When it works, nobody notices. When it fails, the damage is catastrophic. Unmanaged BYOD is essentially running that plumbing without inspections, maintenance, or even a diagram of where the pipes go.
The HIPAA Security Rule
The rule requires covered entities to implement technical safeguards for electronic protected health information (ePHI). Mobile devices must include:
- Encryption
- Authentication controls
- Secure messaging
- Remote wipe capability
- Access logs
When a nurse uses a device enrolled in Mobile Device Management (MDM), the organization can enforce all four. When that same nurse uses an unmanaged personal phone funded by a stipend, the organization is hoping these safeguards exist, not enforcing them.
Managed devices ensure that HIPAA-compliant mobile devices are used across the organization. This creates an auditable security environment.
Under HIPAA, it is the covered entity’s responsibility to safeguard ePHI, not the employee’s. A stipend shifts the cost but not the liability.
BYOD (Bring Your Own Device) Policies
BYOD (Bring Your Own Device) Policies became popular because they reduce hardware costs. However, healthcare environments are not typical workplaces. Sensitive patient data is constantly accessed and shared across devices, which increases security risks.
- Lack of Device Control in Clinical Workflows
When staff use personal devices, hospital IT teams cannot fully enforce critical security measures such as encryption policies, software updates, or device lock settings. This makes it difficult to maintain consistent security standards and meet HIPAA compliance requirements. - Security Threats to Patient Data
Unmanaged devices create additional risks, including screenshots of patient information, use of unsecured messaging apps, and lost or stolen phones. These vulnerabilities can expose sensitive data, and healthcare breaches are among the most expensive in any industry.
What Is Connectivity as a Benefit for Healthcare?
Connectivity as a Benefit(CaaB) is a managed mobility model where healthcare organizations provide employees with pre-provisioned, HIPAA-compliant mobile devices and connectivity instead of stipends. The devices are MDM-enrolled and centrally managed to ensure security, compliance, and consistent nurse mobile access.
A simple analogy: a stipend is like giving a new surgeon a gift card to a hardware store and telling them to buy their own scalpels. CaaB is like handing them a sterilized, hospital-grade instrument tray on their first day. Both approaches put a tool in the surgeon’s hand, but only one meets the standards required for patient safety.
| Feature | Mobile Stipend Model | Connectivity as a Benefit (CaaB) |
|---|---|---|
| Device quality guaranteed | No control over device quality | Curated device catalog approved by IT |
| MDM enrollment at activation | Not enforced | Devices pre-enrolled in MDM |
| HIPAA compliance from day one | Not guaranteed | Encryption and remote wipe enabled |
| Employer visibility into device fleet | No centralized visibility | Single dashboard for device and connectivity management |
| Employee out-of-pocket cost | Often high (stipend rarely covers full cost) | Zero or minimal cost |
| Tax treatment for the employer | Often taxable income for an employee | Treated as a business expense |
| Compliance audit readiness | Limited documentation | Full audit trail and reporting |
The Tax Advantage: IRS Notice 2011-72
When a healthcare organization provides a mobile device and plan for legitimate business reasons, the benefit is treated as a working condition fringe benefit under IRS Notice 2011-72. This means it is excludable from the employee’s gross income and is not subject to payroll taxes.
Read more on how HR and finance teams can manage this transition seamlessly, from provisioning to payroll integration.
A $50 monthly stipend, by contrast, is taxable income. The employee pays income tax and FICA on it, and the employer pays the employer’s share of FICA. For a 5,000-employee health system, the additional payroll tax burden alone can reach six figures annually, all without improving device security or compliance one bit.
Under IRS Notice 2011-72, employer-provided cell phones used for business purposes are treated as a non-taxable fringe benefit. In contrast, cash stipends are considered taxable income for both the employer and the employee.
Case Framework: A 5,000-Nurse Health System
Let us put real numbers behind this. Consider a regional health system with 5,000 nurses and clinical staff currently receiving a $50/month mobile stipend. The annual cost amounts to $3 million.
To understand the financial and operational impact, the table below compares a traditional stipend program with a managed Connectivity as a Benefit (CaaB) model powered by Spenza.
| Metric | Mobile Stipend Model | CaaB with Spenza |
|---|---|---|
| Monthly cost per employee | ~$50 stipend + ~$3.83 employer FICA | ~$28/month (device + data plan with volume pricing) |
| Annual cost (5,000 employees) | ~$3.0M | ~$1.68M |
| HIPAA-compliant devices | Unknown (0% guaranteed) | 100% MDM-enrolled |
| Audit trail for ePHI access | None | Complete audit logs |
| Remote wipe capability | Not available | Enabled for all devices |
| Employee out-of-pocket cost | $30–$60/month beyond stipend | $0 cost to employee |
| Nurse satisfaction / retention impact | Often negative (stipend seen as insufficient) | Positive (perceived as a valuable benefit) |
| Annual savings | — | ~$1.32M saved annually |
For a 5,000-nurse healthcare system, switching from stipends to a managed connectivity program can reduce costs by over $1.3 million annually while improving compliance and device reliability.
The savings come from three sources:
- Elimination of payroll tax on stipends
- Volume-negotiated pricing through Spenza’s marketplace
- Removal of “ghost stipends” paid to terminated employees whose records were not updated promptly.
Beyond the dollars, the impact on hospital employee retention is significant. Nurses who receive a modern, functional device on day one feel supported. Those handed a $50 stipend feel like an afterthought. With the average turnover cost for a bedside RN exceeding $56,000, even a modest improvement in retention pays for the entire CaaB program multiple times over.
The average turnover cost for a bedside RN is about $56,300. A Connectivity as a Benefit (CaaB) program that improves retention by just 2% across a 5,000-nurse health system can save over $5.6 million annually in turnover costs alone.
How Spenza Powers Connectivity as a Benefit (CaaB) For Healthcare

Spenza is a Connectivity-as-a-Service platform that combines telecom expense management, an operator-neutral connectivity marketplace, and full-stack device provisioning into one integrated solution. For healthcare, this translates into a purpose-built CaaB engine.
1. Branded Employee Portal:
Nurses access a health-system-branded portal to select from a curated catalog of approved devices. The experience feels like the organization’s own service, reinforcing CaaB as a genuine benefit rather than a vendor interaction.
This simplifies deployment for both staff and IT teams.
2. MDM Integration:
Every device provisioned through Spenza is automatically enrolled in the organization’s MDM at activation. Encryption, passcode policies, remote wipe, and app whitelisting are configured before the device reaches the employee. This is baked into the workflow, not an optional step.
This ensures:
- Security compliance
- Policy enforcement
- Centralized control
3. eSIM Provisioning:
Spenza uses eSIM technology for instant, over-the-air activation for connectivity. No physical SIM cards to ship, inventory, or swap. A nurse hired on Monday can have a fully activated, compliant device by Tuesday without IT staff touching the phone.
4. Operator-Neutral Marketplace:
The platform is not locked into a single carrier. A multi-site health system with hospitals in urban and rural areas can assign different carrier plans to different locations, all managed from one dashboard and consolidated onto one bill.
5. Telecom Expense Management (TEM):
Spenza’s TEM layer provides real-time visibility into the entire device fleet. Automated alerts flag zero-use devices (a nurse may have left without their line being deactivated) or excessive data usage. The platform can save up to 30% on wireless costs through invoice auditing and plan optimization.
With this Centralized Cost and Usage Management, hospitals gain visibility into:
- Device usage
- Connectivity costs
- Deployment across departments
Conclusion: Why Healthcare Organizations Are Moving Beyond Stipends
Mobile devices are now part of everyday clinical workflows. Yet stipend programs offer little control over device security, reliability, or compliance, creating risks for hospitals and uncertainty for HR and finance teams managing costs.
As healthcare becomes more digital, unmanaged personal devices can lead to inconsistent nurse mobile access, HIPAA exposure, and unclear program spending.
Connectivity as a Benefit provides a more structured approach. By standardizing secure mobile devices and connectivity, healthcare organizations can improve compliance, simplify cost management, and give frontline staff reliable tools for patient care.
For hospital leaders across IT, HR, and finance, the shift is becoming clear: the question is no longer whether mobile connectivity should be managed, but how quickly organizations can move beyond stipend-based models.
FAQs
Connectivity as a Benefit or CaaB is an employer-sponsored mobile program that provides employees with discounted mobile plans and optional devices. Unlike cash stipends, CaaB programs are fully managed, include governance, reporting, and automated billing settlement, and qualify as non-taxable working condition fringe benefits under IRS Notice 2011-72.
Mobile stipends provide little visibility into device security, compatibility, or usage. In regulated environments like healthcare, unmanaged personal devices can expose sensitive patient data. The average healthcare data breach can cost around $9.77 million, making device security and compliance a major priority for hospitals.
Frontline employees using personal stipend-funded devices often face connectivity failures due to old hardware and unreliable plans. CaaB provides employer-vetted enterprise devices with unlimited mobile plans, ensuring secure, reliable connectivity. This eliminates delays in time-tracking, route confirmation, patient charting, and HR document completion.
Yes. Most CaaB programs allow personal use while protecting clinical data. Mobile Device Management (MDM) separates work and personal data through secure containers, ensuring patient information remains encrypted and remotely wipeable without affecting personal content.
Spenza is a platform that delivers managed Connectivity as a Benefit programs. It provides enterprise-grade devices, subsidized unlimited mobile plans, automated billing, reporting dashboards for HR and Finance, and mobile device management integration. Spenza enables organizations to reduce costs, improve workforce productivity, and offer a fully tax-efficient connectivity benefit.
Ready to replace stipends with secure, compliant connectivity? Schedule a free Healthcare Connectivity Assessment with Spenza and receive a custom ROI analysis for your health system.






